Clinical Pearl #13: Post PAO: Common Questions That Can Be Surprising for Patients
When I work with patients after a Periacetabular Osteotomy (PAO), they often ask a lot of questions they didn’t know would be a part of the recovery process. I want to put together a resource for these frequent, and sometimes personal, questions I field. Is urinary frequency after a PAO common? I heard and felt popping and cracking after my PAO, is this normal? Should it be painful to cough, sneeze or laugh after a PAO? The answer to all of these is yes. These are just a few topics we’ll cover.
Urinary Frequency Post PAO
“I’m home from my PAO and I feel like I have to pee all the time…” Sorry to be frank, but yes it is common. However, getting up frequently to use the bathroom, or bedside commode, isn’t the easiest in the early days returning home from the hospital. The amount of time needed to get to the point of relief is longer than you think. And, it can cause anxiety thinking that you won’t make it! For those of you with a prior history of hypertonicity of the lower pelvic floor, the frequency is worse than usual as well.
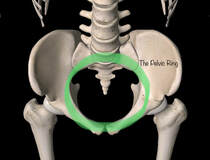
The when the 2 sides of the pelvis come together, they create something called the pelvic ring. This is where a large number of intricate muscles insert. This ring is interrupted with the PAO procedure, and these muscles are all of a sudden pulled or slightly reoriented. Guarding, or spasm, of these muscles is common, thus contributing to the urgency. Planning ahead and even scheduling your bathroom time might help with the anxiety this can cause. This will improve in the first few weeks after surgery. If it doesn’t, consult with your surgeon.
Constipation Post PAO
What about the other side? Early days in the hospital recovering from your PAO will be spent with a pharmacy of medications from pain killers to muscle relaxers, and anti inflammatories, along with other medications prescribed by your physician during your recovery. Due to the amount of anesthesia required for surgery, your system will be backed up. Yes, you will be constipated, and a stool softener will be on your pharmacy list. Constipation can even be quite painful for some. Anesthesia will slow your bowel movements (BMs), and your BMs will be monitored for movement prior to discharge from the hospital. Continuing to monitor this at home is necessary for your overall health and how your system is recovering. By your 2 week follow up with your surgeon, your BMs should be well on the road to normal for you.
Clicking, Popping, or Snapping Post PAO
“I just heard clicking” or “I felt something snap or pop”. After your PAO, sounds and sensations like these are going to happen. Think about how invasive the procedure is, and how much swelling and bleeding happens with the procedure. Over time, swelling will decrease. As you move tissues which previously were full of fluid, these areas can feel and sound like Rice Crispies. These sounds and sensations WILL ALWAYS be shocking and stressful when they first happen. Just about every patient with whom I’ve worked thinks that they just retore the labrum, or something happened with the bone and their healing is doomed. Hold on a minute!! Have faith that your physician did his/her job with the PAO, and know that sitting or mild movement is not enough to undo this skilled work. I always advise when these noises happen, take a second and breathe. Typically, these noises are not painful, but sometimes they can be. The reaction is the same. Breathe, and identify what motion created it. Monitor it. Anytime you have concerns, or something lingers, please consult your physician.
Pain with Coughing, Sneezing, or Laughing Post PAO
“Oh gosh, I don’t want to cough after my PAO!” or “Please don’t make me laugh too hard after my PAO!” With the PAO procedure, the lower abdominals are cut away from where they insert on the iliac crest (upper pelvic bone) and are sutured back in place when the procedure is done.. Forceful abdominal contractions, laughing, sneezing, coughing, and moving in bed, can increase your pain in the lower quadrant of your abdominal area. Many times, your hip flexors will be helping these activities, depending on your position, thus your hip pain can increase as well. During the PAO, at least one hip flexor muscle was cut away and sutured back, and the iliacus (deep muscles on the inside of the pelvis) muscle on the inside of the ilium was pulled away to be able to access the bone for cutting. These muscles have all been traumatized, guarded, and are easily stressed. Quick, forceful activities stress these.
Pain with Lifting Your Leg Post PAO
“I can’t pick up my leg without significant pain” or “How long will I need to lift my leg with my hands?” The reaction of the hip flexors previously noted is directly why. Removing muscle, pulling muscles, retracting muscles, all contribute to trauma and need healing. The weight of your leg is greater than you ever think it is until you recover from hip surgery. Minimize attempting to lift your leg while it is straight getting into and out of bed, and shorten the lever arm of your leg when you can by bending your knee. Yes, you will have to assist with your hands for at least 1-2 months after surgery as you continue to recover.
These are much more common, or last longer, with recovery from a PAO than from a hip scope. It is not uncommon for those with hip scopes to have at least one of these issues above after surgery. Again, this is normal and part of your healing process in the first weeks after surgery. Any time you have concerns about any sensations, do not hesitate to consult your surgeon with these concerns.
Abnormal Menstrual Cycles After Surgery
It is not unusual for your body to have changes to the menstrual cycle after surgery. This can include, but not limited to, spotting, altered cramping, and break throughs. The greater the stress of surgery, the greater the potential for this interruption. The stress can be the extent and severity of the cycle and your body's adaptation to it, or your stress related to the entire event. For those of you in child bearing years, please consult your physician for any questions related to your birth control and effectiveness during this time.
For other references related to preparing for PAO surgery, please refer to #10 Surgical Preparation or #16 Initial Hip Surgical Recovery

